I recently came across some fascinating information about a drug called Dipyridamole and its potential role in treating glaucoma. As you may know, glaucoma is a serious eye condition that can lead to irreversible vision loss if left untreated. Researchers have discovered that Dipyridamole, originally designed as a blood thinner, may also have properties that can help improve blood flow to the eye and reduce intraocular pressure. While more studies are needed to fully understand its effectiveness, this new discovery could potentially lead to a breakthrough in glaucoma treatment. It's always exciting to learn about innovative research, and I can't wait to see how this develops!
Glaucoma treatment: what actually works to protect your vision
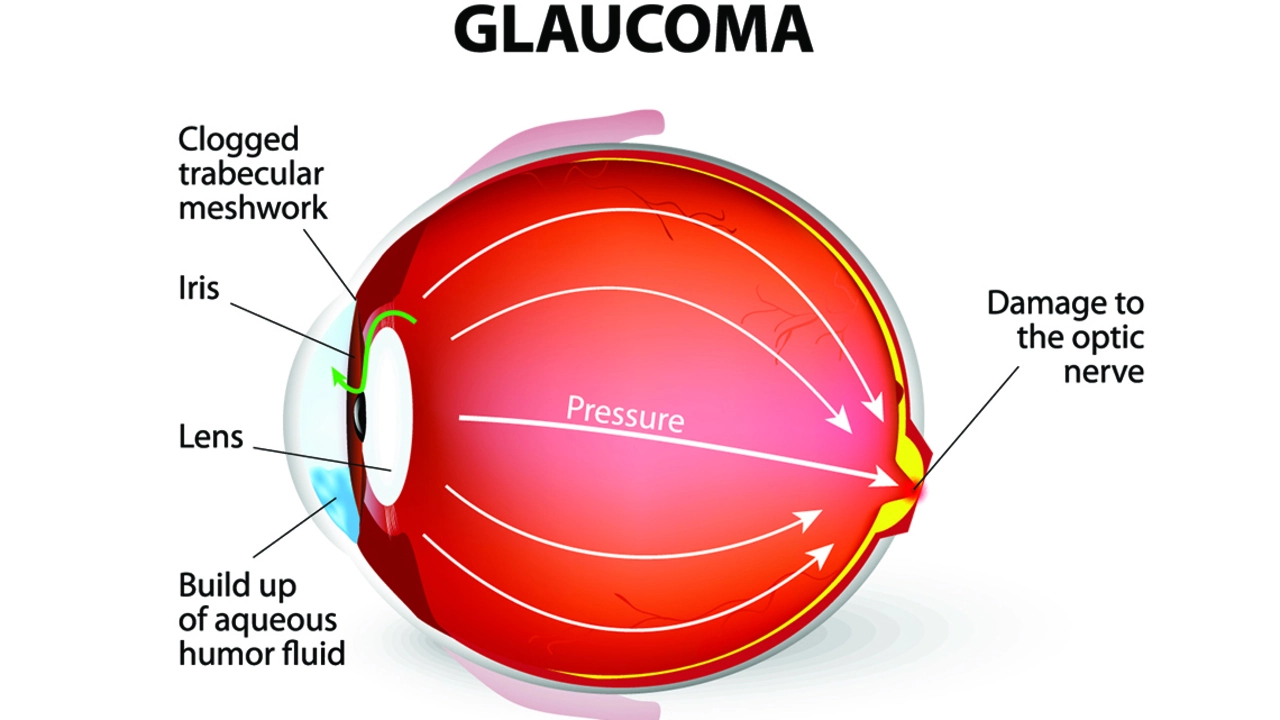
Glaucoma damages the optic nerve, usually because eye pressure is too high. The main goal of treatment is the same in every case: lower pressure and keep your vision. You’ll see a mix of medicines, lasers, and sometimes surgery used together. Below is a clear, practical rundown so you know what to expect and what matters most in day-to-day care.
Common medical and laser options
Eye drops are the first line for most people. They reduce fluid production or improve fluid outflow from the eye. The main classes are:
- Prostaglandin analogs (e.g., latanoprost): usually once daily, strong at lowering pressure. Side effects: darkening of lashes or mild redness.
- Beta-blockers (e.g., timolol): reduce fluid production. They can affect heart rate or breathing in sensitive people, so your doctor will ask about heart and lung issues.
- Alpha agonists and carbonic anhydrase inhibitors: used alone or with others to add pressure control.
If drops aren’t enough or you want fewer meds, selective laser trabeculoplasty (SLT) is a common next step. SLT uses light to improve drainage and can lower pressure for months or years. It’s quick, done in the clinic, and recovery is usually fast.
Surgery is considered when drops and laser don’t control pressure or if damage is progressing. Traditional options like trabeculectomy create a new drainage path. Newer options, called MIGS (minimally invasive glaucoma surgery), are gentler and often used at the same time as cataract surgery.
Practical tips for daily care and follow-up
How you use treatment matters as much as the treatment itself. Use these simple habits to get the most out of therapy:
- Drop technique: tilt your head back, pull the lower lid to make a pouch, place one drop in the pocket, close your eye for 1–2 minutes. Avoid blinking hard—this can push the drop out.
- Wait between drops: if you have two different eye drops, wait about 5 minutes between them so the first one can absorb.
- Reduce side effects: gently press the inner corner of your eye for 1 minute after putting drops (punctal occlusion). This lowers blood absorption and side effects.
- Stick to follow-up tests: intraocular pressure checks, visual field tests, and OCT scans track damage and treatment success. Bring a list of medications to each visit.
- Use reminders: phone alarms, a daily pillbox, or a chart by the sink. Missing doses is a common reason glaucoma progresses.
Tell your doctor about allergies, heart or lung disease, and all medicines you take—some drugs interact with glaucoma meds. If vision changes suddenly, you get severe eye pain, or you notice unexpected side effects, contact your ophthalmologist right away.
Glaucoma is usually a lifelong condition, but with the right treatment plan and regular checks, most people keep useful vision for life. Work with your eye doctor, follow the routine, and ask questions until you feel confident about your care.